
Dan Limmer, BS, NRP

by Dan Limmer, BS, NRP
Our articles are read by an automated voice. We offer the option to listen to our articles as soon as they are published to enhance accessibility. Issues? Please let us know using the contact form.
We hear a lot about the differences between the geriatric patient and younger adult patients. Rather than list the differences between patient types, I’d rather use five of my favorite geriatric calls to highlight some of the important elements.
For additional details and insights I have recorded an audio debrief of each patient (18 mins).
I was called to a patient who was “spitting up blood.” I arrived to find an alert 80-year-old female patient whose skin was pink, warm and dry. These are good signs. She was very concerned about the blood. My clinical challenge was to determine whether it had come from the tracheobronchial tree or from the GI tract. My history questions got me nowhere. I then asked if she could show me a facial tissue that she’d spit blood into. She retrieved one. The “blood” was hot pink. Like Pepto Bismol. So much like it that I asked if she had taken some. Indeed she had, and the mystery was solved.
The lesson: Sometimes it’s obvious—go with it.
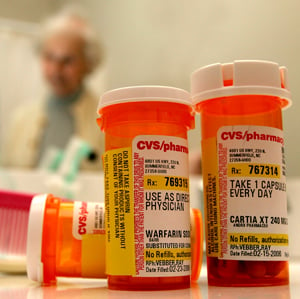
A woman in her 70s was lethargic. Her daughter had come over to check on her and found her “not right.” I found a patient with bradycardia and lethargy. While getting a history and preparing to begin a differential diagnostic approach, I asked about medications. The daughter advised me that she had just brought over a new medicine container for her mother, to help her remember her pills. It turned out that the patient had been going left to right, not up and down, when taking her pills from the container—meaning she had taken her morning medications 4 times a day for the past couple of days. This resulted in her getting a lot more beta blocker than she was supposed to have—and the bradycardia we saw.
The lesson: Medication errors (low dosing and overdosing) are common in the elderly population.
This patient had Alzheimer’s disease and was in an assisted living facility. The call was for an altered mental status. In instances like this, a baseline must be established first and then a differential diagnostic process performed. We ruled out diabetic conditions. We were relatively successful in getting him to perform some components of the stroke scale. All negative.
When I asked the staff about his history, they told me he had recently broken a rib. This made me consider pneumonia as a result of hypoventilation—and therefore sepsis. Pneumonia and urinary tract infections in this population should create a strong suspicion of sepsis.
The lesson: Suspect sepsis in the geriatric patient with altered mental status.
I was dispatched for a man with chest pain in an assisted living facility. I arrived to find him apparently lethargic and sitting on the end of the bed. The staff told me they had given him 9 nitroglycerin tablets. (Gasp!) They were then told by the physician to put him back in bed.
As if this wasn’t enough to make me want to transport him, a dozen staff members stuck their heads in the room to wish him well—more than I had ever seen at this facility. I asked the nurse if the patient was normally more active than this. He was. I decided he needed to go and transported him.
Turns out he was having an MI. The staff and family called to thank me for taking him to the hospital.
The lesson: Changes in mental status are usually significant findings.
This isn’t a clinical point—it was simply a moment in time.
Sometimes in an ambulance you have an experience with a patient that is so moving it becomes the highlight of the call. This patient, a woman in her 80s, had been a nurse in World War II. She’d gone from New York City to North Africa, and she shared with me her experiences with the humility and elegance of that generation. I was honored to be in her presence.
The lesson: You and your patient have one thing in common: You are both people. Never forget that.
The audio above that goes with this post provides more details and additional lessons from these five patients. Please enjoy, and share this post.


Dan Limmer, BS, NRP

Dan Limmer, BS, NRP

Limmer Education
The audio on this article is not working; https://limmereducation.com/article/a-tale-of-five-geriatric-patients/
Hi Colleen- Thanks for letting us know! We have corrected the problem.